By Anne Tumlinson Innovations
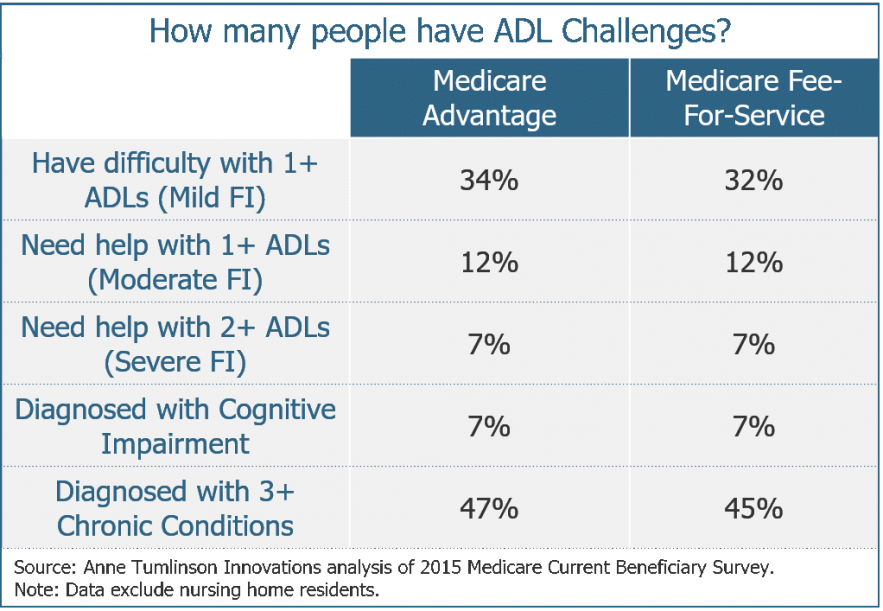
The individual characteristic that contributes most to complex care needs is the inability to function in activities of daily living (ADLs), such as eating, bathing, and dressing. The winners in population health management will be the health plans and providers that figure out how to identify individuals with ADL impairment and address their needs with comprehensive care management and targeted non-medical services.
Emerging Focus on Non-Medical Care Needs
The good news is that more and more health plans and providers are recognizing this and are acquiring and deploying non-medical service capabilities, such as home care. Examples include Humana’s acquisition of Kindred at Home; Anthem’s acquisition of Aspire Health, a palliative care company; and the merger of CVS and Aetna to offer retail-based, person-centered services. These types of partnerships break down silos in the health care industry and allow for a reimagining of service delivery and supports for the complex care population.
This is an exciting trend that contrasts sharply with the historical tendency of the health care sector to view non-medical services and supports as a domain entirely separate from medical care. That’s all changing with the policy imperative to shift payment models from fee-for-service to value-based care and to enable population health management. Further, the Medicare Advantage (MA) population is growing steadily, as is MA enrollment of the complex care population — those with functional impairment (FI) and multiple chronic conditions.
Another important step toward breaking down silos between medical and non-medical care is the Creating High-Quality Results and Outcomes Necessary to Improve Chronic (CHRONIC) Care Act, which was passed as part of the Bipartisan Budget Act of 2018 and signed into law on February 9, 2018.
Among other changes, the CHRONIC Care Act created a new category of supplemental benefits under the Medicare Advantage program: special supplemental benefits for the chronically ill (SSBCI). MA plans now have the option to offer SSBCI, which include non-medical services that have a reasonable expectation of improving or maintaining the health or overall function of the chronically ill enrollee.
These expanded benefits signal an important turning point in Medicare policy. For the first time, Medicare allows coverage of non-medical benefits through the Medicare Advantage program, as well as significant flexibility in terms of who receives these benefits and which services they receive.
Focusing on Functional Impairment
These changes are encouraging, but we need to make sure that health plans and health care providers focus on functional impairment as a critical individual characteristic to target in their population health efforts.
Research shows that having an impairment in ADL functioning is strongly associated with high health care costs, even when holding constant the existence of chronic conditions. Health care costs for individuals with three or more chronic conditions are twice as high when they also have moderate to severe functional impairment.
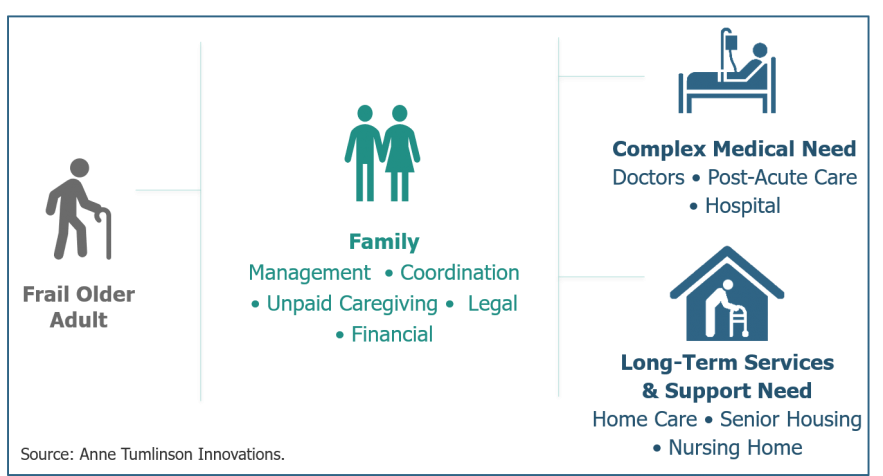
Second, the needs of the population with functional impairment are not being met today. Only about one-third of the seven million older adults with functional impairment are receiving paid long-term services and supports (LTSS) to help them with ADLs. The rest are relying exclusively on unpaid family caregivers for LTSS. These older adults and their family caregivers face tremendous challenges in managing the range of medical care and LTSS they need. In a sense, families remain the only true “accountable care organization” for older adults who need significant levels of medical care and LTSS.
What’s Needed: A Vision for the Future
One of the biggest obstacles to meeting LTSS needs is that the U.S. lacks a comprehensive insurance system to protect older adults against the high costs of care. Family caregivers provide most of the care because there is no way to finance paid care. Another key challenge is that even when individuals have the funds to pay for care, they struggle to find the right care, to coordinate within the context of all their care needs, and to oversee and monitor quality. The LTSS system is largely unmanaged and uncoordinated. This lack of access to and management of LTSS likely contributes to high health care spending.
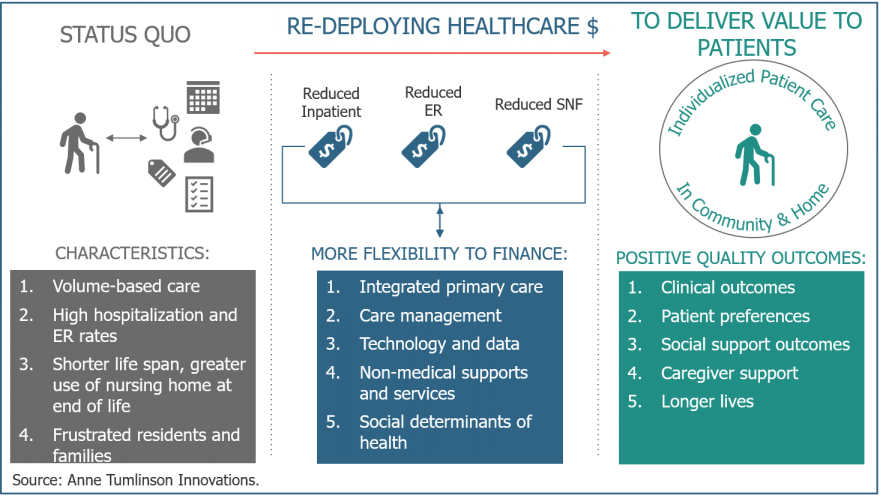
It is time for health plans and providers to step in. They can help in two ways:
- Plans and providers can redeploy inefficient health care spending to the non-medical services (including LTSS) that better meet individual needs.
- They can also coordinate resources and help individuals and families manage the overall care delivery ecosystem. In doing this, they will achieve the goals of reducing health care spending AND improving outcomes for individuals and families.
The key to achieving this vision is in finding and identifying individuals with complex care needs, thoroughly assessing these needs, and intervening in a manner that is consistent with their goals and preferences. Finding these individuals will require plans and providers to get more comfortable screening for and assessing functional impairment.
The policy environment has never been more flexible or encouraging. We cannot wait much longer as the population with complex care needs grows with the aging adult population. The time is now.